If you’re over 40 and experiencing sudden, fleeting double vision, especially at the end of the day, it’s likely not just screen fatigue or ‘getting older.’ The real culprit is often a hidden, lifelong eye misalignment (a latent phoria) that your brain can no longer easily compensate for. This guide investigates the root causes and outlines the specific steps to get an accurate diagnosis and effective treatment.
You’re wrapping up a long day, and suddenly the words on your screen seem to shimmer and split in two. You blink, rub your eyes, and the image snaps back into focus, but a nagging sense of unease remains. This experience—of intermittent double vision, or diplopia—is increasingly common for active adults, especially after the age of 40. The immediate assumption is often digital eye strain or the onset of presbyopia (age-related farsightedness), leading to generic advice like “take more breaks” or “get reading glasses.”
While these factors play a role, they often mask a deeper issue. Many people who experience this frustrating symptom are grappling with a problem that has been dormant for decades. This isn’t about your eyes suddenly failing; it’s about a highly efficient compensation system finally showing signs of fatigue. The key isn’t just to manage the symptoms, but to investigate and understand the underlying mechanism that has just become active.
But what if the true reason for your visual fatigue and fleeting double vision isn’t just about the hours you spend on a screen, but about how your brain has been working overtime your entire life to keep your vision single and clear? This article will explore that very possibility. We will delve into why this phenomenon often surfaces after 40, show you how to perform a simple self-check, compare treatment options, and clarify which specialist holds the key to a lasting solution.
This guide provides a structured investigation into the often-misunderstood world of binocular vision. By following the sections outlined below, you will gain a clear understanding of the potential root cause of your symptoms and the precise actions you can take to find relief.
Summary: Investigating the Causes of Sudden Onset Double Vision
- Why Does Your Latent Phoria Become Symptomatic After Age 40?
- How to Check Your Stereopsis Level With a Simple Finger Test?
- Micro-Prisms or Digital Detox: Which Solves Screen-Induced Diplopia?
- The Misdiagnosis Mistake: Why Binocular Issues Are Often Treated as Migraines?
- When to Stop Driving If You Experience Intermittent Double Vision?
- Why Is the Cover Test Essential for Detecting Lazy Eye?
- Why Does Your Child Skip Lines When Reading Aloud?
- What Does an Orthoptist Do That an Optician Cannot Treat?
Why Does Your Latent Phoria Become Symptomatic After Age 40?
The sudden appearance of double vision after 40 often feels alarming, but in many cases, it’s not a new problem but an old one that has just crossed a symptomatic threshold. The real culprit is frequently a latent phoria, a subtle, natural misalignment of the eyes that you’ve likely had since childhood. For decades, your brain has worked tirelessly behind the scenes, using a powerful mechanism called fusional vergence to fuse the two slightly different images from each eye into a single, clear picture. This compensation is automatic and incredibly effective—until it isn’t.
After age 40, two key factors conspire to overwhelm this system. First, the natural aging process reduces the flexibility of the eye’s lens (accommodation), making focusing at near distances more difficult. This increased effort places an additional demand on the entire visual system. Second, the “stamina” of your fusional vergence reserves can decline. A hospital-based study of pre-presbyopes found a significant link between increased age (even within the 35-40 range) and a recession in the near point of convergence, a key measure of binocular function. Your brain simply runs out of the extra energy needed to keep forcing the eyes into alignment, especially after hours of near work or when you’re tired.
This process is known as decompensation. The underlying phoria hasn’t changed, but your ability to control it has. Research confirms this trend, demonstrating that the prevalence of fusional vergence dysfunction increases from 2.3% in teenagers to 5.4% in the 40-49 age group. This is the moment when the hidden struggle becomes a noticeable symptom, manifesting as eye strain, headaches, and that frustrating, intermittent double vision.
How to Check Your Stereopsis Level With a Simple Finger Test?
While a definitive diagnosis requires a specialist, you can perform a simple at-home test to observe how your eyes work together. This test, often called the “finger sausage” or a basic near point of convergence (NPC) check, gives you a tangible sense of your binocular function and provides valuable information to report to your eye doctor. It helps you move from a vague complaint like “my eyes feel weird” to a specific observation like “I see double when my finger is 6 inches from my nose.”
This test assesses your ability to maintain binocular fusion as an object moves closer. Your two eyes must turn inward (converge) smoothly and in unison to keep the object single and clear. When this system is strained, you might notice one eye struggling to keep up, resulting in blur or double vision.
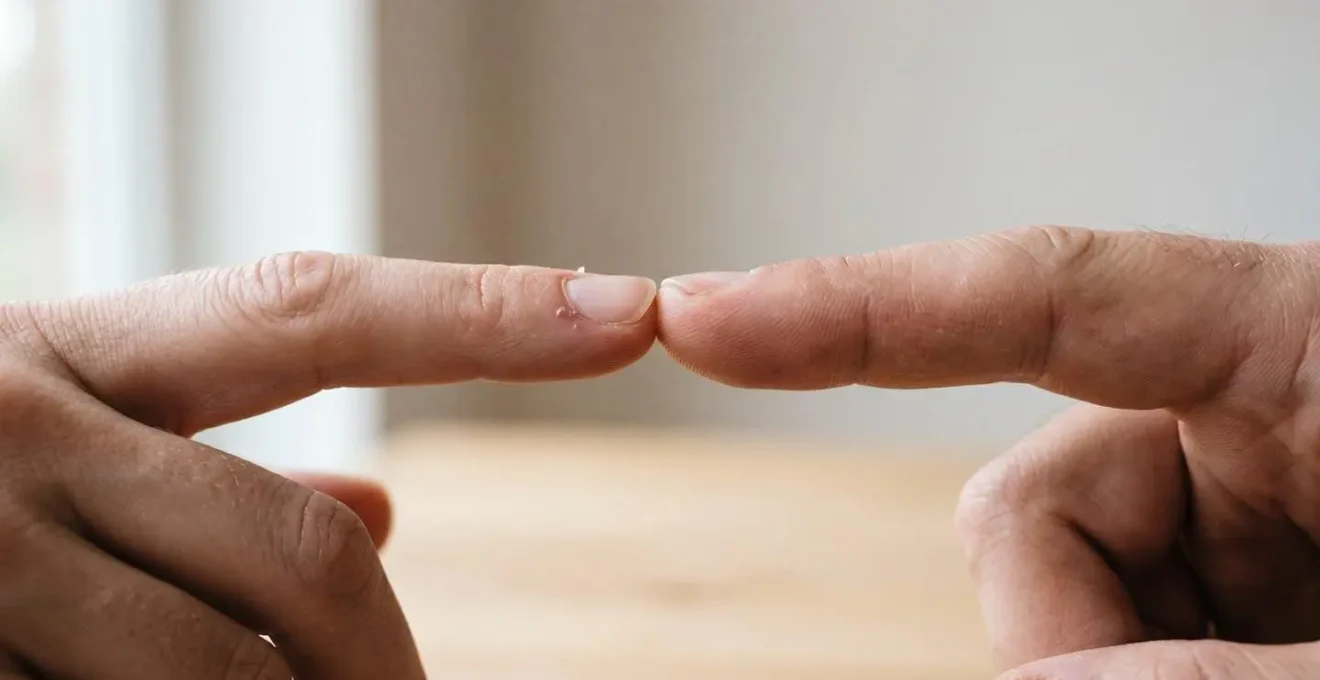
Performing this test allows you to witness your own visual system in action. The point at which you lose the ability to hold a single image is a key indicator of strain on your fusional vergence reserves. Here is a simple protocol you can follow:
- Sit comfortably and hold one finger (or a pen) at arm’s length.
- Focus on the tip of your finger. You should see it as single and clear.
- Slowly begin to move your finger directly towards the bridge of your nose.
- Pay close attention to your finger. The goal is to keep it single for as long as possible.
- Stop the moment you see two fingers (diplopia) or when you feel one of your eyes “give up” and drift outward. This is your “break point.”
- Note the distance from your nose where the break occurred. A break point further than 4-6 inches can be an indicator of convergence insufficiency.
Micro-Prisms or Digital Detox: Which Solves Screen-Induced Diplopia?
When faced with screen-induced double vision, many seek immediate relief, leading to two common but very different approaches: behavioral changes like a “digital detox” and optical aids like micro-prisms. A digital detox involves reducing screen time or following the 20-20-20 rule (every 20 minutes, look at something 20 feet away for 20 seconds). While this can provide temporary relief by reducing the demand on your visual system, it doesn’t address the underlying inefficiency. The symptoms often return as soon as you resume normal activities.
Micro-prisms, on the other hand, are a passive optical solution. These specialized lenses are prescribed to bend light before it enters the eye, effectively tricking the brain into thinking the eyes are properly aligned. This can provide immediate and significant relief from symptoms. However, it’s crucial to understand that prisms manage the problem; they don’t fix it. They act as a crutch, and as the experts at Cook Vision Therapy Center note, they require ongoing dependency. For a deeper understanding, the following table compares these approaches with a third, rehabilitative option: vision therapy.
| Treatment Approach | Mechanism | Timeline | Long-term Effect | Best For |
|---|---|---|---|---|
| Digital Detox | Behavioral avoidance of visual trigger | Immediate symptom reduction | Temporary relief only | Mild, recent-onset symptoms |
| Micro-Prisms | Passive optical realignment of images | Immediate relief | Ongoing dependency required | Significant, disruptive symptoms needing immediate management |
| Vision Therapy | Active neuro-rehabilitation to retrain eye-brain coordination | 4-8 months | Potential permanent correction | Patients seeking to fix root cause and achieve independence |
As the comparison shows, the most appropriate solution depends on your goals. For mild, recent symptoms, a digital detox may suffice. For immediate management of disruptive symptoms, prisms are a powerful tool. However, for those seeking to correct the root cause of the problem—the inefficient eye-brain coordination—vision therapy stands out as the only active, rehabilitative approach designed to retrain the visual system for a potentially permanent fix.
The Misdiagnosis Mistake: Why Binocular Issues Are Often Treated as Migraines?
One of the most frustrating aspects of Binocular Vision Dysfunction (BVD) is its remarkable ability to mimic other conditions, leading to years of misdiagnosis and ineffective treatment. The most common culprit is vestibular migraine, a neurological condition that shares a confusingly similar list of symptoms: overwhelming dizziness, nausea, a feeling of being off-balance, difficulty focusing, blurred vision, and light sensitivity. Many patients suffering from BVD are told they have migraines, anxiety, or vertigo, and they embark on a treatment journey that fails to address the visual root of their problem.
The numbers reveal a startling discrepancy. According to vision specialists, only about 1 percent of the U.S. population has vestibular migraines. In stark contrast, at least 20% of the population suffers from BVD. This suggests a significant number of people are being diagnosed with a rare neurological condition when they may actually be suffering from a much more common, and highly treatable, visual one. The overlap in symptoms arises because a strained visual system sends conflicting information to the brain, disrupting the sense of balance and spatial awareness, just as a migraine can.

This misdiagnosis often happens because a standard eye exam may not include the specialized, prolonged tests needed to uncover a decompensating phoria. If your “migraines” are triggered by visually intensive tasks like driving, shopping in a big-box store, or working on a computer, and if they are not responding to typical migraine treatments, it is a strong signal that an underlying binocular vision issue should be investigated. Getting the right diagnosis is the first and most critical step toward finding real relief.
When to Stop Driving If You Experience Intermittent Double Vision?
While most cases of fatigue-induced double vision are not life-threatening, the implications for activities like driving are serious and must not be ignored. Driving requires rapid, seamless shifts in focus between the road ahead, your dashboard, and your mirrors. A struggling binocular system can fail during these critical moments, turning a quick glance into a moment of disorientation or double vision, which can be acutely dangerous.
It’s essential to self-assess your risk honestly. A useful way to think about this is a “Traffic Light Model” for risk. At the “Green” level, your symptoms are minimal and predictable, appearing only after very long stretches of driving. “Yellow” signifies a higher risk, where double vision appears when you change focus, such as checking your mirrors. This is a clear sign to limit driving and seek an urgent evaluation. “Red” is a medical emergency.
If sudden double vision occurs with specific warning signs, treat it as a medical emergency. Certain neurological symptoms that appear with double vision are major red flags. These include sudden weakness or numbness on one side of your face or body, trouble speaking or slurred speech, confusion, loss of balance, or severe dizziness.
– Refocus Eye Doctors, Sudden Double Vision: Causes, Diagnosis, and Management
If you experience any of the “Red” symptoms described above, do not drive. Have someone take you to the emergency room immediately to rule out a stroke or other acute neurological event. For “Yellow” or “Green” symptoms, the responsible action is to schedule a comprehensive binocular vision exam as soon as possible and, in the interim, take frequent breaks and avoid driving at dusk or in other challenging visual conditions.
Why Is the Cover Test Essential for Detecting Lazy Eye?
The term “lazy eye” (amblyopia) is often used colloquially, but in a clinical setting, an eye care professional must differentiate between various types of eye misalignments. The single most important diagnostic tool for this is the cover test. This simple but powerful test is the gold standard for revealing how your eyes are truly aligned and how they behave when they are not forced to work together. It’s what allows a specialist to distinguish between a tropia (a constant, visible misalignment) and a phoria (a latent, hidden misalignment that only appears when one eye is covered).
During a cover test, the doctor has you fixate on a target while they cover one of your eyes. They are watching the uncovered eye for any movement. Then, they watch the eye that was just uncovered to see if it moves to re-align with the target. This “cover-uncover” and “alternating cover” process reveals the presence, direction, and magnitude of any misalignment. As described in diagnostic protocols from institutions like NYU Langone, this test is fundamental in assessing binocular diplopia.
For an adult experiencing intermittent double vision, the cover test is crucial because it makes the latent phoria visible. When one eye is covered, it relaxes to its natural, misaligned position. When uncovered, the doctor can see it “snap” back into place as your brain re-engages its fusional vergence to create a single image. This observable movement is the definitive proof of the underlying issue and allows the specialist to measure the degree of misalignment using prisms, which is the first step toward determining the best course of treatment, whether it be prisms or vision therapy.
Why Does Your Child Skip Lines When Reading Aloud?
While this article focuses on adult-onset symptoms, the roots of Binocular Vision Dysfunction often trace back to childhood. If you’ve ever noticed a child skipping lines when reading, losing their place, or complaining that words are “moving,” you may have been witnessing the early signs of a condition like convergence insufficiency (CI) or saccadic dysfunction. These are the very same foundational issues that can decompensate and cause double vision in adulthood.
Saccades are the rapid, precise eye movements we use to jump from one word to the next while reading. In saccadic dysfunction, these movements are inaccurate and jerky, causing the reader to overshoot or undershoot their target word, resulting in skipping or re-reading lines. Convergence insufficiency, as discussed, is the inability to comfortably maintain eye alignment for near tasks. For a child, this makes the act of reading physically exhausting. Instead of seeing one clear, stable line of text, their eyes are constantly fighting to keep the words from blurring or splitting apart.
This is not a rare problem. In fact, clinical studies document that the prevalence of convergence insufficiency in school-age children can be as high as 13%, with a commonly cited figure around 5%. Many of these children develop compensatory strategies, like tilting their head or using a finger to track words, and their issue goes undiagnosed. They grow into adults with a seemingly “cured” problem, but the underlying inefficiency remains, waiting for the added stresses of aging and digital device use to trigger a decompensation decades later.
Key Takeaways
- Your sudden double vision is likely not a new issue, but the decompensation of a hidden, lifelong eye misalignment due to age and visual stress.
- Simple self-tests can help document symptoms, but a definitive diagnosis requires a specialized cover test to measure the latent phoria.
- The ultimate solution often lies beyond prisms or digital detox, focusing on neuro-rehabilitative vision therapy provided by a specialist.
What Does an Orthoptist Do That an Optician Cannot Treat?
Navigating the world of eye care can be confusing. You might have an optician who fits your glasses, an optometrist who performs your annual check-up, and an ophthalmologist who treats eye diseases. However, when the problem is not the health of the eye or the optical prescription but the coordination between the eyes and the brain, you need a different kind of specialist: an orthoptist or a behavioral optometrist. These professionals are like physical therapists for the eyes.
An optician’s role is to dispense corrective lenses based on a prescription—they do not diagnose or treat vision conditions. A standard optometric exam is excellent for checking eye health and determining your glasses prescription, but it may not include the in-depth testing required to quantify a binocular vision disorder. An ophthalmologist is a medical surgeon focused on disease and surgery. While they are essential for ruling out pathological causes of double vision, they typically do not oversee vision therapy for functional issues.
The orthoptist is the specialist who lives in this gap. They are experts in diagnosing and treating disorders of binocular vision, eye movements, and eye alignment. They administer specialized, prolonged tests to measure your fusional reserves and pinpoint the exact nature of your phoria decompensation. They are uniquely equipped to treat conditions like Convergence Insufficiency, Saccadic Dysfunction, and Accommodative Infacility, often without surgery. A major clinical trial demonstrated that 73% of children with convergence insufficiency improved their reading and reduced symptoms after just 12 weeks of office-based vision therapy, proving its effectiveness. For an adult, this means a path toward actively retraining your visual system rather than just passively compensating with prisms.
Your Action Plan: Finding the Right Eye Care Specialist
- Optician (The Framer): Visit them to fit and adjust glasses based on a prescription. Do not expect diagnosis or treatment of your double vision from them.
- Optometrist (The GP of Eyes): Start here for a comprehensive eye health exam to rule out disease and get an updated glasses prescription. Specifically ask them if they perform binocular vision testing.
- Ophthalmologist (The Surgeon): Your optometrist will refer you to an ophthalmologist if they suspect an underlying disease, tumor, or neurological issue is causing your symptoms.
- Orthoptist/Behavioral Optometrist (The Physical Therapist for Eyes): This is your target specialist. Seek a referral or find one directly if you suspect BVD. They are the experts who diagnose and treat the specific conditions (like Convergence Insufficiency) that cause functional double vision.
- Evaluate Your Diagnosis: If your diagnosis is “migraine” or “anxiety” but your symptoms are primarily visual and task-related, insist on a binocular vision evaluation with a specialist from the fourth category.
If you are experiencing the frustrating symptoms of intermittent double vision, headaches, and visual fatigue, do not dismiss them as an inevitable part of aging. Take the proactive step of seeking a comprehensive binocular vision assessment from an orthoptist or a behavioral optometrist. A correct diagnosis is the key that unlocks effective, targeted treatment and offers the potential for a permanent solution.