Blog
Vision is often taken for granted until it falters or gradually deteriorates. Maintaining optimal eye health extends far beyond the simple act of reading letters on an illuminated chart. It is a comprehensive discipline that encompasses everything from understanding the nuances of a routine screening to navigating the complex world of refractive surgery and dynamic visual processing. The eyes act as a direct window to overall systemic health, making their care a critical component of holistic wellness.
This comprehensive resource is designed to demystify the various facets of ocular care. Whether it involves deciphering a complex clinical prescription, evaluating the right time to visit an emergency department, or understanding why 20/20 vision does not always equate to perfect sight, the information provided here serves as a foundational pillar. By exploring these vital topics, individuals are empowered to make informed, confident decisions regarding their optical health and daily visual comfort.
Navigating Routine and Emergency Eye Examinations
The cornerstone of long-term ocular health is the professional eye examination. While the convenience of online vision checks has grown, these digital tools only offer basic refractive estimates and completely bypass the crucial medical evaluation of the eye’s internal structures. Relying solely on virtual screenings carries the significant risk of missing asymptomatic conditions like glaucoma or early macular degeneration.
What to Expect During Standard Screenings
A standard 20-minute clinical appointment involves an intricate series of diagnostic tests. Optometrists do not merely determine if glasses are required; they meticulously examine the retina, optic nerve, and blood vessels. The standard two-year interval between these tests is widely recognized as a non-negotiable benchmark in healthcare. This timeframe allows practitioners to track minute physiological changes before they manifest as noticeable visual impairments, ensuring early intervention when necessary.
Recognizing Ocular Emergencies
Understanding when a symptom requires an immediate visit to A&E rather than a routine check-up is a critical skill that can literally save an individual’s sight. Standard appointments are sufficient for gradual vision changes, but emergencies demand urgent medical protocols.
- Sudden, painless loss of vision in one or both eyes.
- Severe ocular pain accompanied by nausea or a severe headache.
- Chemical exposure or foreign bodies deeply embedded in the eye.
- A sudden onset of flashing lights or a dense shadow falling over the field of vision.
Managing Common Eye Infections and Allergies
Red, swollen, or irritated eyes are among the most frequent reasons individuals seek medical advice. However, accurately identifying the root cause—whether viral, bacterial, or allergic—is essential for applying the correct treatment protocol. A distinct gritty sensation often points toward an infection, whereas persistent, overwhelming itchiness is typically the primary hallmark of an allergic reaction.
Safe At-Home Remedies and Persistent Myths
Before contacting a GP, specific home interventions can provide substantial relief, provided they are scientifically sound. For instance, applying a cold compress offers immediate relief for allergic pink eye by constricting the superficial blood vessels, thereby rapidly reducing swelling and soothing the itch. Conversely, widespread cultural remedies must be approached with caution. The popular myth of placing warm, used tea bags on an infected eye is highly counterproductive; the porous nature of the bag and the moisture create an ideal breeding ground for bacteria, which can severely worsen a localized infection.
Correct Application of Clinical Treatments
When medical drops are prescribed, applying them correctly to heavily swollen eyes can be challenging. Proper technique involves tilting the head back and gently pulling the lower lid downward to create a small pocket. This ensures the active medicinal compound rests against the conjunctiva, maximizing absorption without causing further physical trauma to the inflamed eyelids.
Demystifying Your Optical Prescription
To the untrained eye, an optical prescription resembles a complex mathematical equation. However, decoding these clinical values is crucial for anyone intending to purchase corrective lenses or understand the progression of their visual acuity.
Decoding the Numbers: Spheres, Cylinders, and Axis
Every standard prescription follows a universal formatting language that dictates the precise curvature of the required lens.
- Locate the Sphere (SPH) value to identify the primary refractive error. Minus signs (-) indicate myopia (short-sightedness), while plus signs (+) denote hyperopia (long-sightedness).
- Check the Cylinder (CYL) metric to determine the presence and severity of astigmatism, which indicates an irregular curvature of the cornea.
- Note the Axis number, a value between 1 and 180. This provides the exact rotational angle for the astigmatism correction. It is completely normal for this axis to shift by a few degrees over time as the eye naturally ages.
- Look for the Add power, which calculates the additional magnification required for reading or close-up tasks, typically affecting individuals experiencing presbyopia.
The Importance of Prescription Validity Rules
Optical prescriptions are not valid indefinitely. They carry an expiration date, universally set at two years, due to the gradual but constant physical changes in the eye’s anatomical structure. Attempting to use an expired prescription for new glasses forces the brain and intrinsic ocular muscles to overcompensate. This physiological strain directly leads to asthenopia (severe eye strain), chronic headaches, and potentially faster deterioration of visual comfort.
Evaluating Laser Eye Surgery Options
For individuals seeking long-term freedom from corrective eyewear, refractive surgery offers highly transformative results. However, modern advertising often promotes heavily discounted pricing, such as exceptionally low per-eye costs, which rarely reflect the comprehensive care or advanced technology required for complex corrections. Candidacy must be determined through rigorous clinical assessment, not marketing appeals.
Assessing Candidacy and Pre-Surgical Requirements
The foremost deal-breaker for any laser candidate is corneal thickness. Think of the cornea as the structural foundation of a house; the laser must reshape this tissue to correct vision while leaving a sufficiently thick, stable base to prevent long-term complications. Furthermore, candidates must provide clinical evidence that their prescription has remained completely stable for a minimum of 12 months. Hormonal fluctuations, notably those experienced during pregnancy and after breastfeeding, temporarily alter corneal hydration and curvature, mandating a strict waiting period before surgery can be safely considered.
Comparing Procedures: LASIK, SMILE, and Surface Ablation
Advancements in ophthalmic technology mean that a one-size-fits-all approach no longer exists. Surgeons select the procedure based on the patient’s unique anatomical profile and daily lifestyle.
- LASIK: The most widely performed procedure, offering incredibly fast visual recovery through the creation of a precise corneal flap.
- SMILE: A keyhole, minimally invasive alternative. It is highly favored by professionals because it severs fewer corneal nerves, resulting in significantly less post-operative dry eye compared to traditional methods.
- Surface Ablation (PRK): The safest designated alternative for individuals whose corneas are too thin to safely accommodate a LASIK flap, though it requires a longer healing timeline.
Beyond 20/20 Acuity: The Role of Dynamic Vision
A common misconception is that achieving 20/20 vision on a standardized chart equates to flawless sight. In reality, visual processing encompasses how rapidly and accurately the brain interprets continuous visual stimuli. The static clinical chart is merely a photograph, whereas everyday life requires the brain to act as a high-speed video processor.
Understanding Visual Processing and Contrast Sensitivity
Standard examinations frequently overlook dynamic vision deficiencies. An individual might effortlessly read the bottom line of a static chart in a brightly lit room, yet struggle immensely with moving objects or experience debilitating glare during night driving. In low-light environments, high contrast sensitivity—the ability to distinguish an object from its background—becomes far more critical than pure visual acuity. Advanced custom wavefront technologies in modern surgery and specialized lenses aim to address these subtle imperfections, offering enhanced night vision precision.
Enhancing Peripheral Awareness and Reaction Times
Visual reaction time dictates how quickly the muscular system responds to visual cues, a vital metric for competitive gaming, sports, and safe driving. By proactively training peripheral awareness, individuals can expand their functional field of view. This training not only improves reflex speeds but also effectively reduces symptoms of motion sickness by better aligning visual processing with the inner ear’s vestibular feedback system.
Ultimately, comprehensive optical care is an ongoing journey of education and proactive management. By understanding the intricacies of clinical screenings, the precise science behind prescriptions, and the technological marvels of modern surgery, individuals are better equipped to protect their most vital sensory asset for a lifetime.
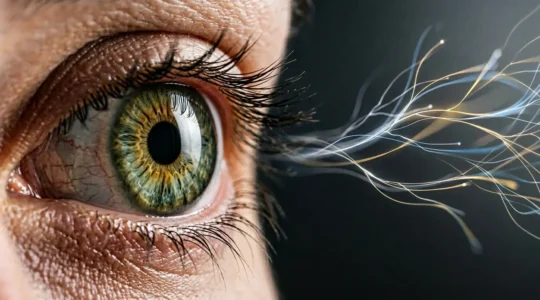
Is 20/20 Vision Enough? Why Visual Processing Matters More Than Acuity?
The common belief that 20/20 vision equals perfect vision is a myth; your brain’s ability to process dynamic information is far more critical for real-world…
Read more
LASIK vs. SMILE: Which Surgery Offers the Fastest Recovery for Professionals?
For a busy professional, the best laser eye surgery isn’t just about the fastest recovery; it’s about matching the procedure’s biomechanics to your specific performance…
Read more
Am I Suitable for Laser Eye Surgery With a High Astigmatism Prescription?
Your high astigmatism isn’t an automatic disqualification, but your corneal thickness and prescription stability are the real, non-negotiable gatekeepers for surgery. Suitability is a mathematical…
Read more
How to Read Your NHS Optical Prescription Without Being an Optometrist?
In summary: Your prescription decodes your vision: a plus (+) sign is for farsightedness, while a minus (-) sign is for nearsightedness. The CYL and…
Read more
Pink Eye Remedies: What Works at Home Before Calling Your GP?
Most pink eye is treatable at home, but using the wrong remedy can cause serious harm or delay necessary medical treatment. Allergic versus infectious pink…
Read more
NHS Eye Tests: What Actually Happens During Your 20-Minute Appointment?
Contrary to popular belief, your NHS eye test’s primary purpose is not just to get a glasses prescription. It is a comprehensive health check that…
Read more