
Most pink eye is treatable at home, but using the wrong remedy can cause serious harm or delay necessary medical treatment.
- Allergic versus infectious pink eye requires different approaches; a cold compress that soothes an allergy can be insufficient for a bacterial infection.
- Common folk remedies like tea bags are non-sterile and dangerous, carrying a proven risk of introducing severe fungal or bacterial infections into the eye.
Recommendation: Your first step is not treatment, it’s triage. Correctly identify your specific symptoms to understand when to self-care safely and when to see a doctor immediately.
Waking up to a red, itchy, and swollen eye is an unwelcome and often alarming experience. Your first instinct might be to search for quick home remedies, a search that often unearths a mix of sensible advice and dangerous myths, like using tea bags or questionable herbal poultices. As a pharmacist, my priority is to guide you towards safe and effective self-care, and crucially, to help you understand when home treatment is no longer appropriate. The most valuable remedy is not a compress or a drop, but knowledge—the ability to perform a simple triage on your own symptoms.
This isn’t just about finding relief; it’s about understanding the underlying cause. A gritty, sticky eye points to a different origin than an intensely itchy, watery one. One might be a highly contagious bacterial infection, while the other is a simple allergic reaction. Treating them the same way is ineffective at best and harmful at worst. This guide is designed to empower you with a pharmacist’s perspective: to move beyond generic advice and learn to read your body’s signals, apply genuinely helpful remedies correctly, and, most importantly, recognize the clear red flags that demand an immediate call to your GP or a visit to A&E.
This article provides a structured approach to managing pink eye at home. We will break down the distinct sensations and what they mean, detail the correct, safe application of remedies, explain hygiene protocols to prevent spreading, and provide a definitive checklist of symptoms that signal a medical emergency.
Summary: A Pharmacist’s Triage Guide for Pink Eye
- Why Do Cold Compresses Provide Immediate Relief for Allergic Pink Eye?
- How to Apply Eye Drops Correctly When Your Eyes Are Swollen?
- Itchy or Gritty: Which Sensation Confirms It’s Just an Allergy?
- The Tea Bag Myth: Can Placing Tea on Your Eye Worsen the Infection?
- When Does a Red Eye Become a Medical Emergency Requiring A&E?
- Why Does Mascara Become a Bacterial Breeding Ground After 3 Months?
- Why Does Dry Air Break Down Your Protective Tear Film So Quickly?
- Bacterial or Viral Conjunctivitis: How to Stop the Spread in Your Household?
Why Do Cold Compresses Provide Immediate Relief for Allergic Pink Eye?
A cold compress provides rapid relief from the intense itching and swelling of allergic conjunctivitis through a simple physiological mechanism: vasoconstriction. When you have an allergic reaction, your body releases histamine, causing blood vessels in the eye to dilate and leak fluid. This leads to the characteristic redness, swelling, and watery discharge. The cold temperature causes these tiny blood vessels to constrict, or narrow, which reduces blood flow to the area. This action directly counteracts the effects of histamine, decreasing redness, alleviating swelling, and calming that maddening itch.
This remedy is most effective for allergic or viral pink eye, where inflammation is the primary issue. It’s less helpful for bacterial conjunctivitis, where the problem is an active infection that requires a different approach. The key is that the relief is symptomatic; it manages the discomfort but doesn’t cure the underlying allergy. The effectiveness of this simple home treatment is supported by clinical evidence; a 2013 randomized clinical trial found that cold compresses combined with artificial tears reduced hyperemia (redness) more effectively than other treatments. For it to be both safe and effective, however, proper application is essential to avoid skin damage or introducing new contaminants.
Your Action Plan: Safe Cold Compress Application Protocol
- Use a clean washcloth soaked in cold water, wrung out so it’s not dripping.
- Do NOT apply ice or a frozen pack directly to the eyelid to avoid the risk of frostnip or tissue damage.
- Limit the application to 10-15 minutes at a time, with breaks in between to allow the skin to return to normal temperature.
- Apply gentle pressure over closed eyelids; never press directly on the eyeball itself.
- Use a fresh, clean cloth for each application to prevent any risk of bacterial contamination.
How to Apply Eye Drops Correctly When Your Eyes Are Swollen?
Applying eye drops to a swollen, irritated eye can be challenging, but correct technique is vital to ensure the medication is effective and to prevent further irritation or contamination. The goal is to deliver the drop into the conjunctival sac—the small pocket created by pulling down your lower eyelid—without the dropper tip ever touching your eye, eyelid, or lashes. This ‘no-touch’ rule is the most important principle of sterile eye drop administration. Contaminating the bottle tip can introduce bacteria, turning a helpful remedy into a source of secondary infection.
When your eyes are swollen, it may be harder to create this pocket. Lying down or tilting your head far back uses gravity to your advantage, stabilizing your hand and head. Gently pulling the lower lid down creates the necessary space. After instilling the drop, it’s equally important to close your eye gently (not squeezing it shut, which forces the drop out) and apply light pressure to the inner corner near your nose. This technique, called punctal occlusion, blocks the tear duct for a minute or two, keeping the medication on the eye’s surface where it’s needed and preventing it from draining into your throat, which can cause a bitter taste and reduce effectiveness.
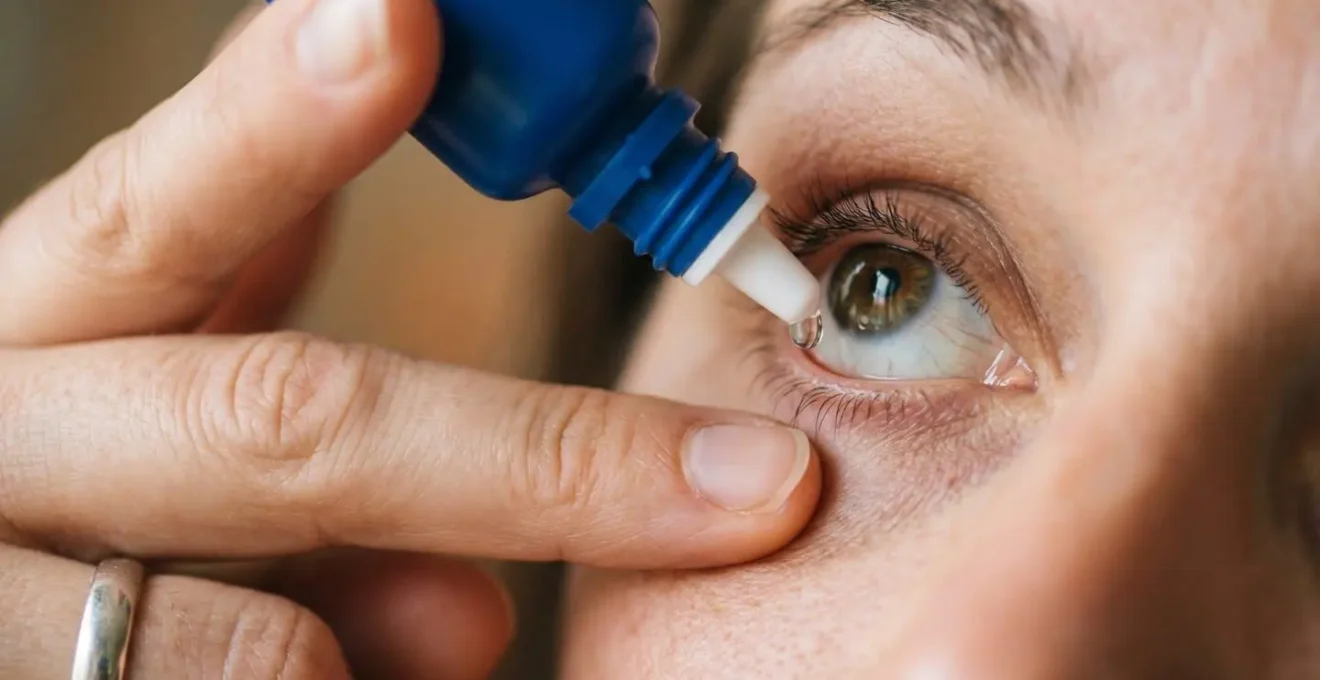
As the image above illustrates, maintaining a small distance between the dropper and the eye is crucial. The following steps, recommended by the American Academy of Ophthalmology, provide a clear, safe protocol for anyone to follow, ensuring each drop counts and your recovery is not compromised by improper technique.
Your Action Plan: Step-by-Step Eye Drop Application
- Wash your hands thoroughly with soap and water before handling eye drops.
- Tilt your head back or lie down flat on your back for stability.
- Gently pull your lower eyelid down with one finger to create a ‘pocket’ for the drop.
- Hold the dropper tip about 1 inch above your eye, ensuring it does not touch the eye or eyelid.
- Look up and squeeze the bottle gently to release one single drop into the pocket.
- Close your eye gently and press your finger on the inner corner (tear duct) for 1-2 minutes to maximize absorption.
- Never touch the dropper tip to any surface and recap the bottle immediately to prevent contamination.
Itchy or Gritty: Which Sensation Confirms It’s Just an Allergy?
The primary sensation you feel is one of the most reliable clues for a preliminary self-triage of pink eye. While a doctor’s diagnosis is definitive, understanding the difference between “itchy” and “gritty” can help you determine the likely cause and appropriate first steps. An intense, overwhelming itch is the hallmark of allergic conjunctivitis. This is often accompanied by clear, watery, or stringy discharge and typically affects both eyes simultaneously after exposure to an allergen like pollen, dust, or pet dander.
In contrast, a gritty, sandy feeling, as if something is in your eye, strongly suggests an infectious cause. If this gritty sensation is paired with a thick, yellow or green pus-like discharge that causes your eyelids to stick together, especially upon waking, bacterial conjunctivitis is the most likely culprit. This type often starts in one eye and can spread to the other. Viral conjunctivitis, the third common type, often presents with a burning or irritated feeling and watery discharge, and is frequently accompanied by symptoms of a common cold. The table below, based on guidance from the American Academy of Ophthalmology, breaks down these key differentiators to help you better assess your symptoms.
| Symptom Type | Primary Sensation | Discharge Characteristics | Eyes Affected | Likely Cause |
|---|---|---|---|---|
| Allergic Conjunctivitis | Intense itching | Clear, watery, or stringy discharge | Both eyes simultaneously | Allergen exposure (pollen, pet dander, dust) |
| Bacterial Conjunctivitis | Gritty, sandy feeling | Thick, yellow or green discharge; eyelids stick together | Often starts in one eye, may spread to other | Bacterial infection |
| Viral Conjunctivitis | Burning, irritation | Watery discharge; minimal mucus | Usually starts in one eye, spreads to other | Viral infection (often with cold symptoms) |
The Tea Bag Myth: Can Placing Tea on Your Eye Worsen the Infection?
Absolutely. The long-standing myth of placing a used tea bag on an irritated eye is not just ineffective; it is actively dangerous and can turn a minor irritation into a severe, vision-threatening infection. As a pharmacist, this is one of the home remedies I most strongly advise against. The core problem is simple: tea bags are not sterile. They are manufactured in an environment designed for food products, not medical ones, and can harbor bacteria and fungi from the soil where the tea was grown. Placing this non-sterile object on a compromised eye, whose natural defenses are already down, is like opening a door for new pathogens.
The warmth and moisture of a damp tea bag create an ideal breeding ground for these microbes to multiply. Furthermore, the fine particulate matter from the tea itself can get into the eye, causing mechanical abrasion on the cornea and worsening inflammation. The risks are not merely theoretical. A harrowing case study documented a patient who developed a deep stromal fungal keratitis after a green tea bag used as a compress ruptured over his eye. This severe fungal infection required 10 months of intensive treatment and resulted in permanent corneal scarring and reduced vision. This extreme but real example underscores the potential for catastrophic harm from a seemingly benign home remedy.
Case Study: Fungal Keratitis Following Green Tea Bag Application
A 29-year-old healthy patient developed deep stromal fungal keratitis in his left eye two weeks after using a green tea bag as a warm compress for meibomian gland dysfunction. The tea bag ruptured over his eye, introducing fungal contamination. Treatment required topical and intrastromal voriconazole injections for 10 months, resulting in permanent corneal scarring and reduced vision. This case demonstrates that tea bags, despite being economical and accessible, are not sterile and carry significant risk of introducing bacteria, fungi, or particulate matter directly into a compromised eye.
Scientific literature further reinforces this caution. As one study on the safety of poultices noted:
tea bags are not sterile and can harbor bacteria, fungi, or particulate matter
– Reevaluating the safety of chamomile poultices in ophthalmic care study, PMC Journal Article on Chamomile Safety
When Does a Red Eye Become a Medical Emergency Requiring A&E?
While most cases of pink eye are minor and resolve on their own or with simple care, it is absolutely critical to know how to distinguish them from a true medical emergency that could threaten your vision. A standard red, itchy, or gritty eye is an irritation; the symptoms on the following list are red flags that indicate a more serious underlying condition like acute glaucoma, keratitis, or uveitis. If you experience any of these, you must stop all home remedies and seek immediate medical attention from an ophthalmologist or at the nearest A&E department.
The most important differentiators are severe pain and changes in vision. The discomfort from common conjunctivitis is typically a surface-level irritation, burning, or grittiness. A deep, aching, or throbbing pain inside the eye is a major warning sign. Similarly, any sudden decrease in vision, blurry vision that doesn’t clear with blinking, or seeing halos around lights is not a symptom of simple pink eye and requires urgent evaluation. High sensitivity to light (photophobia) so intense that you cannot comfortably open your eyes in a normally lit room is another serious red flag. Do not wait to see if these symptoms improve; time is critical in preserving vision when these conditions arise.
Your Action Plan: Red Flag Checklist for Immediate Medical Attention
- Sudden change or complete loss of vision in one or both eyes.
- Severe, deep, aching eye pain (not just surface irritation or grittiness).
- High sensitivity to light (photophobia) that makes it difficult to open eyes in normal lighting.
- Seeing halos or rings around lights, especially at night.
- A chemical splash or a foreign body that feels lodged in the eye.
- The combination of moderate to severe eye pain occurring together with blurred vision.
- Symptoms that are getting significantly worse, not better, after 3-4 days of home care.
- Intense redness in one eye combined with a fever or the eye swelling completely shut.
Why Does Mascara Become a Bacterial Breeding Ground After 3 Months?
Mascara becomes a high-risk bacterial breeding ground due to its unique combination of environment, application, and composition. The mascara tube is a dark, moist, and enclosed environment—the perfect incubator for bacteria to thrive. Every time you use the wand, you introduce microorganisms from your skin and eyelashes into this tube. This process, called inoculation, is unavoidable. The wand then returns to the tube, delivering a fresh batch of bacteria to the nutrient-rich formula. Over time, the preservative system in the makeup, designed to keep it safe, becomes overwhelmed and breaks down, allowing the bacterial population to grow exponentially.
The recommended three-month disposal rule is not arbitrary; it’s a safety deadline based on studies of cosmetic contamination. After this period, the risk of contaminants like *Staphylococcus aureus* or *Pseudomonas aeruginosa* reaching dangerous levels increases dramatically. Using old mascara is essentially painting a bacterial culture directly onto your eyelashes, millimeters from your eye’s delicate surface. If you have an active pink eye infection, any makeup you use becomes heavily contaminated immediately. Continuing to use that product guarantees you will re-infect yourself, trapping you in a cycle of irritation and infection. This is why a post-infection cosmetic purge is not just recommended, it is medically necessary.

Maintaining strict cosmetic hygiene is a non-negotiable part of eye health. After recovering from any eye infection, it is critical to start fresh to avoid a recurrence. This means discarding any product that came near your eyes during the infection and adhering to the recommended replacement schedules for all eye makeup.
Your Action Plan: Post-Pink Eye Purge and Cosmetic Hygiene Checklist
- THROW AWAY: Any mascara, liquid eyeliner, or cream eyeshadow used during or just before the infection period.
- THROW AWAY: Your contact lens case and the specific bottle of contact lens solution used during the infection.
- THROW AWAY: Any eye makeup that has been open for more than 3 months, paying attention to the Period After Opening (PAO) symbol.
- SANITIZE: All makeup brushes used near the eyes with soap and warm water, then allow them to air dry completely.
- SANITIZE: Eyelash curlers and any other metal tools with a 70% isopropyl alcohol wipe.
Why Does Dry Air Break Down Your Protective Tear Film So Quickly?
Dry air, common in centrally heated homes, air-conditioned offices, and airplanes, acts like a sponge, pulling moisture from any available surface—including your eyes. Your eyes are protected by a thin, three-layered coating called the tear film. Its outermost layer is oily, which prevents the watery middle layer from evaporating too quickly. Dry, low-humidity air accelerates this evaporation process, breaking down the protective oily barrier. As the tear film thins and destabilizes, dry spots can form on the surface of your cornea. This not only causes the familiar symptoms of dry eye—stinging, burning, and redness—but it also leaves your eye more vulnerable to allergens and infectious agents.
When you are focused on a task, like reading or using a computer, your blink rate can drop by more than 50%. Blinking is the mechanism that replenishes and spreads the tear film across the eye’s surface. Reduced blinking combined with a dry environment is a perfect storm for tear film breakdown. This is why symptoms often feel worse at the end of a long workday in an office or after a long drive with the car’s heating on. Taking proactive steps to manage your environment and modify your habits can provide a crucial “environmental shield,” preserving your tear film and reducing irritation, which is especially important when your eyes are already compromised by an allergy or infection.
Your Action Plan: Environmental Shield for Tear Film Protection
- Use a humidifier in your bedroom and workspace to maintain indoor humidity between 40-50%.
- Apply the 20-20-20 rule during screen time: every 20 minutes, look at something 20 feet away for 20 seconds to reset your blink rate.
- Direct car vents, fans, and HVAC airflow away from your face to reduce direct evaporative stress.
- Make a conscious effort to blink fully and frequently during prolonged periods of concentration.
- Consider using preservative-free artificial tears 3-4 times daily to supplement your natural tear film, especially in dry environments.
- Position your computer screen slightly below eye level; this causes your eyelids to be slightly more closed, reducing the exposed surface area of the eye.
Key takeaways
- Triage first: An intense itch with watery discharge points to an allergy (use a cold compress). A gritty feeling with thick, colored discharge points to an infection (contact your GP).
- Never use non-sterile items on your eyes. Folk remedies like tea bags are dangerous and have been proven to cause severe, vision-threatening fungal and bacterial infections.
- Severe pain, any change in vision, or extreme light sensitivity are not symptoms of simple pink eye. They are red flags for a medical emergency that requires an immediate visit to A&E.
Bacterial or Viral Conjunctivitis: How to Stop the Spread in Your Household?
When dealing with infectious conjunctivitis (bacterial or viral), your focus must shift from just personal relief to rigorous household quarantine. Both types are highly contagious and spread through direct contact with eye secretions. An infected person touches their eye and then a doorknob, a remote control, or a tap. The next person to touch that surface can then easily transfer the virus or bacteria to their own eye. Therefore, stopping the spread is a matter of breaking this chain of transmission through meticulous hygiene and creating a ‘patient-only’ zone for personal items.
This involves designating specific towels, washcloths, and pillowcases for the infected individual and washing these items daily in hot water (at least 60°C/140°F) to kill the pathogens. High-touch surfaces throughout the home should be wiped down daily with a disinfectant. Handwashing is the single most important defense; it must be done frequently and thoroughly with soap and water for at least 20 seconds, especially after touching the face or applying eye drops. It is crucial to understand the different contagious periods: bacterial pink eye is generally considered non-contagious 24 hours after antibiotic drops have been started. However, viral pink eye can remain contagious for up to 2 weeks, even as symptoms start to improve. This long contagious window for the viral form requires sustained vigilance to protect the entire household.
Your Action Plan: Household Quarantine Protocol
- Designate a patient-only face towel and hand towel; ideally, switch the entire household to disposable paper towels during the infection.
- Wash the patient’s pillowcase, towels, and bed linens daily in hot water (minimum 60°C/140°F) and detergent.
- Wipe down high-touch surfaces daily: doorknobs, taps, light switches, phones, and TV remotes.
- Never share towels, eye makeup, eye drops, or any item that touches the face.
- Practice rigorous handwashing: use soap and water for 20 seconds after touching the eyes or face, before eating, and after applying medication.
Your vision is invaluable. While this guide provides a framework for safe home management, it does not replace a professional medical diagnosis. If you have any doubt about your symptoms, if they are not improving, or if you experience any of the red flag warnings, the safest and most responsible action is always to consult your GP or a local pharmacist for a direct evaluation.